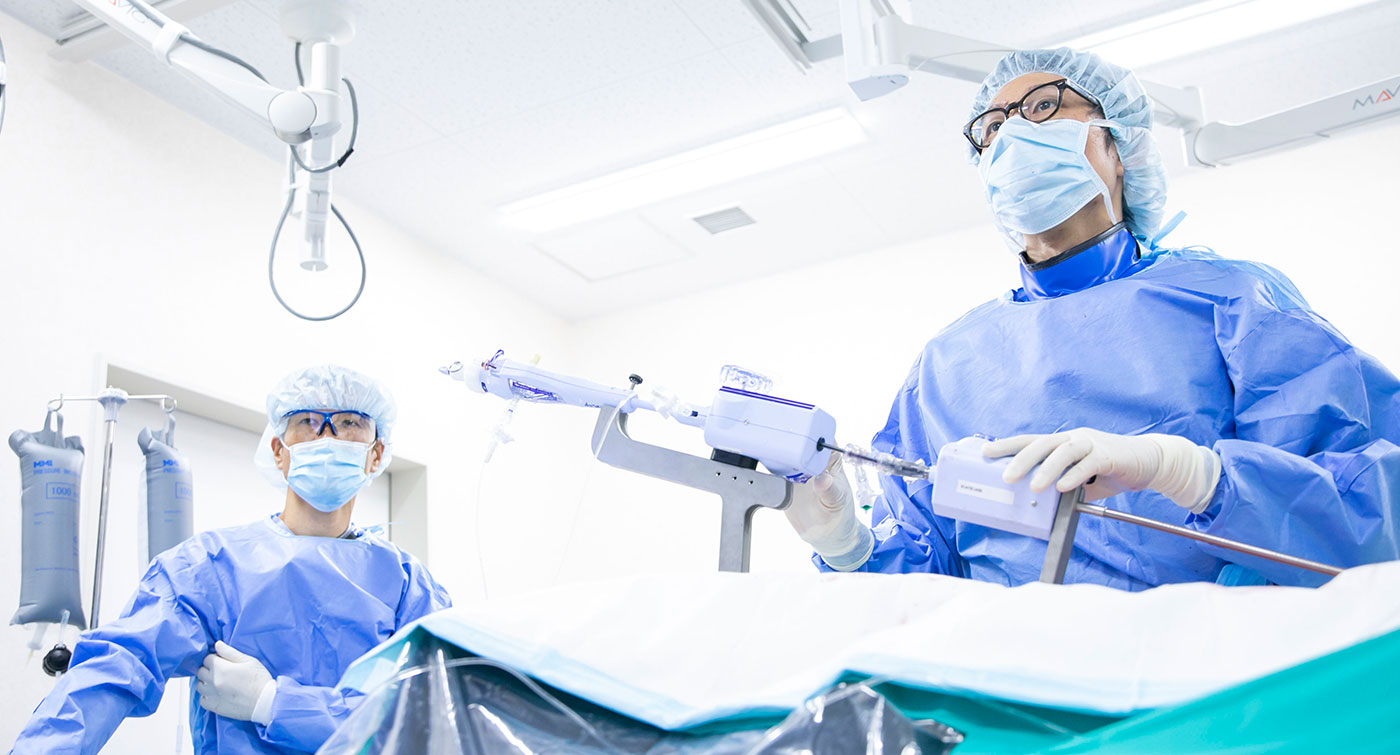
Catheter-based treatment for valvular heart disease — including TAVI for aortic stenosis
and MitraClip for mitral regurgitation — is performed at Kishiwada Tokushukai Hospital
by a specialist certified in both balloon-expandable (Sapien) and self-expanding (CoreValve) TAVR systems,
working within a Heart Team of cardiologists and cardiovascular surgeons.
With 149 TAVI procedures in 2024, this programme represents a high procedural volume within the Osaka region.
For suitable patients, treatment can be performed without open-heart surgery.
TAVI — transcatheter aortic valve implantation
Aortic stenosis occurs when the aortic valve narrows and restricts blood flow from the heart.
In its severe form, it causes breathlessness, chest pain, and syncope,
and carries a high risk of sudden death if left untreated.
TAVI replaces the diseased aortic valve using a catheter passed through the femoral artery —
without opening the chest. It is performed under general or local anaesthesia,
typically with a hospital stay of several days.
TAVI is suitable for patients across a wide range of surgical risk, depending on individual assessment.
Our TAVI specialist holds certification as a TAVR proctor for both
the balloon-expandable Sapien valve and the self-expanding CoreValve system —
meaning he is authorised to train other operators in these techniques.
This dual certification is held by only a limited number of cardiologists in Japan.
All TAVI candidates are evaluated through a Heart Team pathway involving both
cardiology and cardiovascular surgery.
CT imaging and echocardiography are used to assess valve anatomy and confirm suitability.
MitraClip — transcatheter mitral valve repair
Mitral regurgitation occurs when the mitral valve fails to close properly,
causing blood to leak back into the left atrium.
Severe mitral regurgitation leads to progressive heart failure symptoms
including breathlessness, fatigue, and fluid retention.
MitraClip repairs the mitral valve using a catheter introduced through the femoral vein.
A clip is placed on the valve leaflets to reduce regurgitation — without open surgery.
The procedure is typically performed under general anaesthesia.
MitraClip is beneficial for patients who are not suitable for open surgery
due to advanced age, reduced cardiac function, prior cardiac surgery, or other comorbidities.
It is also used for functional mitral regurgitation when symptoms persist despite optimal medical therapy.
- Primary (organic) MR: Structural abnormality of the valve. Considered when surgical risk is high.
- Secondary (functional) MR: Due to ventricular or atrial enlargement. Considered when symptoms persist despite medication.
Suitability is confirmed by transoesophageal echocardiography and Heart Team review.
Diagnostic workup is typically completed on an outpatient basis within one to two weeks.
Surgical options
For patients who are suitable for open surgery, valve repair and replacement
is performed by the Cardiovascular Surgery team at the same hospital,
including minimally invasive robotic MICS using the da Vinci system.
The Heart Team evaluates each case and recommends the most appropriate approach.
For patients from overseas
Patients awaiting TAVI or MitraClip in their home country are welcome to contact us.
Echocardiography reports, CT data, and cardiac catheterisation results
can be reviewed prior to your visit.
Assessment and treatment planning are typically completed within weeks of initial contact.
Transfer from another hospital for pre-procedure assessment and MitraClip treatment is also possible,
including patients requiring inpatient stabilisation before the procedure.
Please provide: echocardiography reports (including transoesophageal echo if available),
CT scan data (DICOM preferred), cardiac catheterisation reports,
and prior treatment records. A referral is helpful but not required.
Appointment
Appointments are required in principle. A referral letter from another medical institution is recommended but not mandatory.
For appointment requests and language support, please see the
Cardiology page.
